The enthusiastic voice on the phone gave us directions the way people in many parts of Latin America do: “Go past the flower market,” she instructed, as we slowly drove down a street lined with stalls full of buckets of roses, daisies and sunflowers. Once we turned right, then left, then left again at the freshly plastered concrete wall, we would find the unpaved road, she said. “The house at the end of that road, that’s us.”
We arrived at Violeta Chuc Sam’s family home in the mountain town of Quetzaltenango, Guatemala, on a breezy Saturday morning in February. Chuc Sam, whose vivacious personality matched the voice giving directions, greeted us at the door. A few weeks earlier she had agreed to welcome our group of journalists to learn more about her mother Francisca Violeta Sam Colop. We wanted to talk about Sam Colop’s long struggle with skin cancer and her fight to access the medication Keytruda.
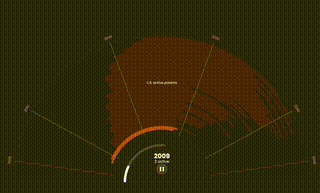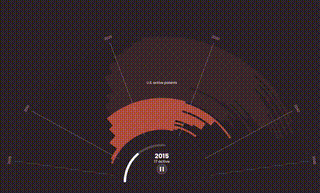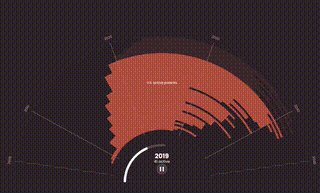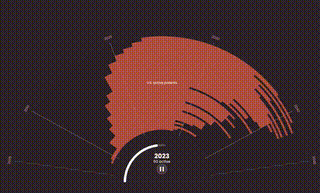
This reporting trip was part of the Cancer Calculus, an investigation by the International Consortium of Investigative Journalists and 47 media partners, including the colleagues I was traveling with, reporter Jody García and photographer Laura Garcia from Guatemalan independent outlet Plaza Pública. Our team spent months examining the global consequences of the exorbitant prices of Keytruda, a novel cancer immunotherapy, known generically as pembrolizumab. It is the bestselling drug in the world, and has made around $163 billion in revenue for its maker, Merck & Co., since its U.S. launch in 2014.

I first came across Sam Colop’s name last August in a 2021 court order granting her access to Keytruda, which she could not afford out-of-pocket. By the time I found her case, I’d already been reviewing numerous similar judicial cases and would go on to find dozens more in the months ahead. But Sam Colop’s case stayed with me. In 2012, she was diagnosed with advanced melanoma, the same illness for which Keytruda was used to put former U.S. President Jimmy Carter in remission. She was an Indigenous Maya K’iche’ educator, a poet and researcher, and an advocate for the preservation of her people’s language and culture. I got excited about the possibility of telling the story of an extraordinary person, beyond what the court records could show. But then, another result appeared in my search: a brief obituary, dated July 5, 2025. Sam Colop was present in the legal document but the possibility of hearing from her was gone.
Months later, I was in her living room, as her daughters Violeta and Marina, and her widower, Juan Chuc Xum, sat below a large framed photo of a stoic Sam Colop reminiscing. Some of the books she authored — a K’iche’ and Spanish children’s version of the Popol Wuj (the sacred text of the Maya people) and her last collection of poems — were neatly arranged on a table nearby. I listened as they took turns telling her story. She was 65 when she died, but younger at heart, Marina joked. She loved to read, sing and dance, and always had a new project going on, Violeta said. She “always likes to be well put together,” said Chuc Xum, still speaking about his wife in the present tense. In 2021, an oncologist outside her government-run insurance system prescribed Sam Colop Keytruda, which by then was a standard treatment for advanced skin cancer in many countries. But her insurer wouldn’t cover the drug. Like thousands of people across Latin America, she had to go to court to force the insurer to do so.

Despite the lack of transparency surrounding prescription drug pricing, our investigation revealed that the cost of Keytruda varies widely by country and even by regions and health systems within a country. A year of treatment can cost anywhere from $29,000 in Indonesia to $130,000 in Colombia, to $208,000 in the United States. In Guatemala, a country with modest income levels, the treatment costs nearly $11,000 per infusion every three weeks, or about $180,000 a year.
“Who could pay for that?” Chuc Xum told us, raising his hands, palms open, before answering his own question. “No one.”
Our reporting began far from the field. For months, we filed and sifted through hundreds of public records, analyzed global data and dug up court documents, to trace the real cost of Keytruda and the corporate maneuvers to maintain its high price and exclusivity. After finding hundreds of cases like Sam Colop’s in Latin America, I learned that a consequence of the high cost is that insurers and hospitals in several countries — with over-stretched healthcare budgets and little negotiation power with Big Pharma — largely won’t provide the medication, unless following court orders. The records quickly raised a broader question: What is it like when a medicine exists, but remains effectively out of reach for those who need it most?
I went to Guatemala to try to answer that question, where the lack of access to Keytruda for both insured and uninsured people seemed glaring.

When I found Sam Colop’s case, her family had been in mourning for just a month after her death. My colleague Jody García reached out to them and we patiently waited until they were ready to talk. The Saturday we visited Sam Colop’s family, they gathered at her house for the interview, as they used to do almost every weekend for family meals. But in a private moment, Violeta, the youngest daughter, told me that in the months since her mother’s passing, it had become rare for them to meet there. “It feels empty without my mom,” she said, almost in a whisper.
After winning her court case, Sam Colop received Keytruda for two years, though periodic shortages meant she sometimes went without treatment. Had she received the medication as scheduled, or even years earlier, her family wonders, would she still be alive? But as we found in our investigation, geography often shapes who has access to expensive and potentially lifesaving medication.
Marina said she finds comfort in knowing her mother prepared them in anticipation of her death, even leaving instructions in her final book of poems. Violeta said she still feels anger over her mother’s death and knows it will take time to accept it. Chuc Xum went down the list of habitual things he misses (seeing her at home, their conversations, going for a stroll — or for dinner — on a random weeknight) until he arrived at what he mostly longs for: growing old with his life partner.
Playing God
In January, Jody García called me with the type of news that excites investigative reporters. She had received a response to a public record request. Some of the details were eye-opening.
A few months earlier, as part of a freedom of information campaign for our investigation, we asked Guatemala’s ministry of health how many patients receive subsidized Keytruda through the public health system. Part of the answer came in a sobering letter written by oncologist Julio Ramírez, the director of the oncology unit at the public hospital in Quetzaltenango, one of only three such units in the country.
Ramírez wrote that only one patient was being provided Keytruda, “not because this is the only indication but because during these almost two years we have only been able to use it in one patient due to the availability [of the drug].” He had received approval for two more treatments, he wrote. Now he had to decide which among his many patients to give it to.
On paper, this was just a data point. Three patients to add to a list. But it signaled so much more: How the decisions of the head oncologist at the public hospital in the country’s second-largest city are shaped by scarcity.

As journalists’ access to public records worsens worldwide, obtaining revealing documents feels increasingly like a small victory. Still, Ramirez’s letter didn’t answer the logical question that followed: How do you decide who receives a drug like this when you don’t have enough for everyone?
In global debates, Keytruda was discussed in terms of pricing strategies, patents, and billion-dollar revenues. It appeared in policy papers and pharmaceutical earnings calls, and in headlines about novel scientific discoveries. But in the oncology unit of this public hospital, the conversation was anything but abstract.
Just after sunrise on a Friday in early February, we met Ramírez, 50, in a small office off a crowded ward, where patients wait their turn in plastic blue chairs lining the hallway. He wore superhero-themed scrubs and had a full head of black hair, marked by a streak of white at the front. His voice rose with excitement when he told the story of the oncology unit, which opened 16 years ago, and where he sees about 40 patients per week.

Access to Keytruda was just one of many needs, he told us, while holding a list of medications he routinely requests for his patients, knowing he isn’t likely to get them all due to budgetary constraints. He said he understood those limitations, especially with high-cost drugs like Keytruda. “It is super expensive … There is no system that can sustain that,” he said. “I wouldn’t be able to pay for it. If I ever needed it, I would have to seek legal protection as well.”
That he was now able to give the medication free of cost to three patients was an improvement, Ramírez insisted.
“But how do you decide who to give it to?” I asked him.
“What’s left for me to do? To play God,” he answered, his voice slightly flustered.
His answer took me aback. Perhaps I expected a winding, technical explanation about biomarkers, efficacy and cost-effectiveness. Instead, I got the instinctive response of someone in a nearly impossible situation. He gave the medication to the first patient who arrived, whose diagnosis and test results indicated they were a good enough candidate, Ramírez said. “That’s all I can do.”
Miles to survive
On that same trip in February, we met the first patient Ramírez treated with Keytruda at the regional hospital. In 2022, Alberto Xum, 65, was diagnosed with metastatic kidney cancer that spread to his lungs. In 2024, when Ramírez got the first approval to provide Keytruda, Xum was at the front of the line. He began infusions in February 2024. By the time we met, he was about to complete his two-year treatment.
Every three weeks, he’d board a bus at 3 a.m. to travel to the hospital in Quetzaltenango to get tests and lab results. Then he’d spend the night at a nearby hotel and go back the next morning for his Keytruda infusion before heading home.

The return trip to his hometown of Samayac should take about two and a half hours, but is often longer depending on roadworks, traffic, and delays in public transport. It took us nearly four hours to get there — with one of those hours stuck in a standstill while a bridge was being repaired.
Finally, we met Xum and his family outside a massive, weekend-long event at their Christian church near the center of the small town. He greeted us warmly and opened up quickly, as if he had been waiting to tell his story. He is an uninsured artisan who makes leather hats and souvenirs.
Xum told us that in 2024, he was ready to give up treatment altogether because he could no longer afford a previous medication (which costs almost $2,000 every three months). When Ramírez told him that he would be able to get Keytruda, and that he wouldn’t have to pay, Xum said he dropped to his knees.
“A doctor alone does not prescribe that, it has an enormous value,” he told us, convinced there was divine intervention. “This is not human. This comes from above.”

Keytruda has shrunk Xum’s tumors, but he’s not in remission. He lives with side effects like skin rashes and constant diarrhea that sometimes force him to get off the bus to use the bathroom on long journeys, like when he goes to art festivals where he sells his products. Then he has to wait for another bus. But he is grateful to have the cancer under control, he told us.
My reporting in Guatemala was shaped by distance. The physical distance patients like Xum cross every few weeks to reach treatment. The legal distance in cases like Sam Colop’s, where access moves through court systems that can authorize care without guaranteeing its consistency.
In Guatemala, those distances are not abstract. There, we found what doesn’t come through in records: small, crowded oncology wards, hours-long travels on deteriorating roads, and the quiet endurance of families still wondering if they could have had more time with their loved ones.